2. Key Challenges and Gaps in Kerala’s Health System
Gaps in Health Policy Framework
Although Kerala published a State Health Policy in 2019 (in Malayalam), the document is not available in the public domain and has not been operationalised through an updated, comprehensive policy framework. This absence is increasingly concerning given the scale and complexity of health challenges facing the state.
Kerala is experiencing rapid population ageing, with nearly 16% of residents aged over 60 years, alongside a high and growing burden of non-communicable diseases and injuries. Diabetes prevalence is estimated at around 20%, mental health conditions affect over 11% of the population—exceeding national averages—and road traffic injuries claim more than 4,000 lives annually.
At the same time, the state faces emerging and re-emerging infectious disease threats, as highlighted during the COVID-19 pandemic, increasing privatisation of healthcare (particularly in maternity care), climate-related health risks, and rising human–animal conflict.
Despite these converging pressures, Kerala currently lacks an updated and publicly articulated Health Policy that responds to present-day realities and is explicitly aligned with Sustainable Development Goal 3 and Universal Health Coverage (UHC) commitments. The absence of such a policy has resulted in a fragmented strategic landscape, with no clear, overarching vision to guide system-wide reforms, prioritisation, and long-term investment in health and well-being.
In the absence of a comprehensive health policy, the state’s response has largely relied on programme-based initiatives such as the Aardram Mission. While such initiatives have contributed to service delivery improvements, they function as implementation programmes rather than as substitutes for a coherent policy framework.
Programme-led approaches, when not anchored within an overarching health policy, risk reinforcing fragmentation and limiting progress towards UHC by focusing on discrete interventions rather than system-wide transformation.
Kerala enacted the Kerala Public Health Act in 2023, which provides a legal framework for public health regulation and enforcement. However, the Act does not constitute a health policy and does not articulate a comprehensive vision for health system development, financing, equity, or accountability, nor does it explicitly recognise health as a human right.
To date, the state has not issued a formal justification for the absence of an updated, comprehensive Health Policy, despite repeatedly referencing programmes such as the Aardram Mission, expansions under government-funded insurance schemes (KASP, MEDISEP), and the Public Health Act as proxies for policy direction.
A comprehensive Health Policy is essential to define strategic priorities, clarify governance and accountability arrangements, integrate public and private sectors, address emerging health risks, and guide sustainable financing and workforce planning.
The continued absence of such a policy undermines coherence, transparency, and public confidence, and limits the state’s ability to respond systematically to Kerala’s evolving health challenges.
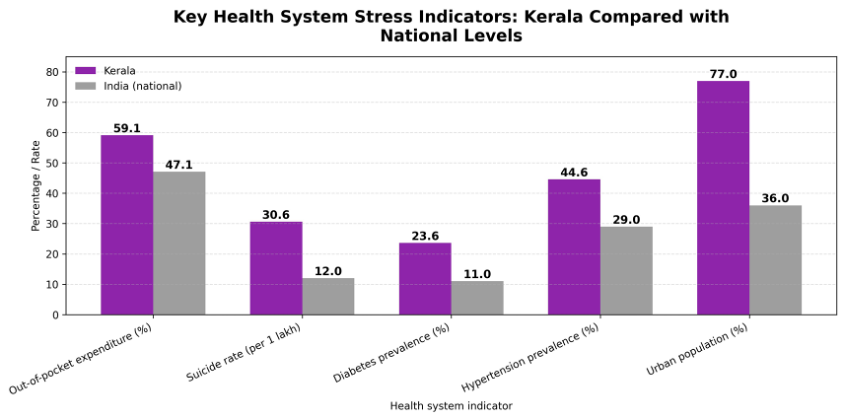
2.1 Disease Burden and Emerging Health Risks
Communicable Diseases
- Diarrhoeal diseases: Kerala reported 5.25 lakh cases of acute diarrhoeal disease in 2025, with 10 deaths (As per state surveillance data – IDSP, 2025). This sustained burden reflects persistent gaps in water quality and sanitation. Seasonal outbreaks continue to strain Primary Health Centres (PHCs), highlighting persistent gaps in sanitation infrastructure and disease surveillance.
- Hepatitis A: In 2025, the state recorded 19,297 suspected cases and 12,378 confirmed cases, with 69 deaths. Outbreaks remained concentrated in districts such as Malappuram and Ernakulam, with adult populations disproportionately affected. Despite vaccine availability, Hepatitis A is not part of the routine immunisation programme, underscoring gaps in targeted vaccination, drinking water safety, and sewage management.
- Chickenpox: Kerala reported 29,055 confirmed chickenpox cases in 2025, with 10 deaths. Suspected cases are not reported separately. The absence of the vaccine from the national immunisation schedule has contributed to recurrent outbreaks, particularly among school-age children, placing avoidable pressure on primary care services.
- Tuberculosis (TB): Over 21,500 new TB cases were identified in 2023, with approximately six deaths reported daily. While Kerala has made notable progress in TB control, drug-resistant TB and high comorbidity with diabetes continue to pose challenges, placing sustained pressure on diagnostic, treatment, and follow-up capacity.
Non-Communicable Diseases (NCDs)
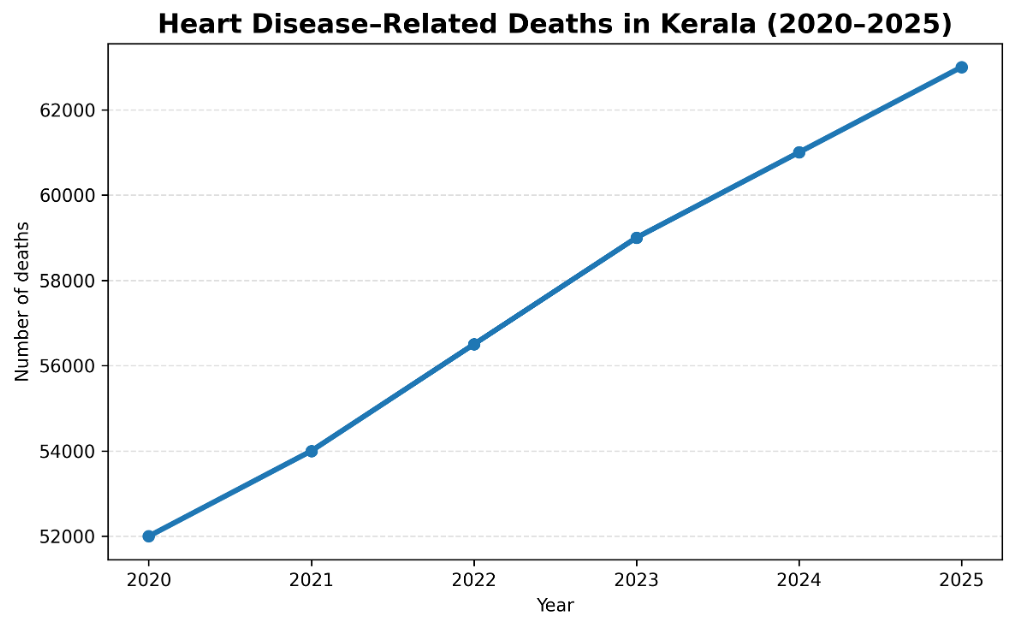
- Cardiovascular diseases: Heart attacks and strokes are the leading causes of death in Kerala, accounting for 26 percent of all deaths. Ischemic heart disease is the top contributor to early mortality, followed by stroke. Alarmingly, 60 percent of male and 40 percent of female cardiac deaths occur before the age of 65. Recent studies also show that 25 percent of heart attack victims in Kerala are under the age of 30, indicating a growing crisis of premature cardiovascular disease.
- Diabetes mellitus: An estimated 23.6% of adults in Kerala live with diabetes, while 18.1% have pre-diabetes, nearly double the national average, positioning the state among the highest-burden settings for diabetes in India (ICMR-INDIAB study). The rising prevalence has increased complications such as kidney failure, heart disease, and amputations, increasing the cost and complexity of care. The system faces growing demand for insulin, dialysis, and patient follow-up, while preventive strategies such as nutrition and physical activity remain under-addressed.
- Hypertension: Approximately 44.6% of adults in Kerala have hypertension, with a substantial proportion remaining undiagnosed or inadequately controlled (ICMR-INDIAAB study). These gaps in detection, treatment adherence, and follow-up contribute to preventable cardiovascular events, including heart attacks and strokes.
- Cancer: Kerala has recorded a 54 percent increase in cancer cases over the past decade, from 39,672 in 2015 to 61,175 in 2024. Thiruvananthapuram reports one of the country’s highest breast cancer rates. Common cancers include breast, oral, lung, and colorectal types. As incidence rises, the public health system is under growing pressure to expand screening, enhance treatment capacity, and reduce the financial burden on families.

- Obesity and lifestyle risks: Sedentary behaviour, unhealthy diets, and physical inactivity are driving obesity and related metabolic disorders. Kerala has emerged as the state with the highest prevalence of abdominal obesity, affecting an alarming 65.4 percent of women. Though often under-recognised, obesity is a growing public health issue in the state, among adults, adolescents, and children. It is closely linked to rising rates of diabetes, hypertension, and heart disease. Preventive and lifestyle-modification efforts remain uneven and under-scaled.
Vector-borne and Zoonotic Threats
- Dengue fever: In 2025, Kerala reported 29,300 suspected dengue cases and 10,886 confirmed cases, with 56 reported deaths. Seasonal surges are straining vector control systems and hospital capacity as urbanisation and climate change create favourable breeding conditions for mosquitoes.
- Leptospirosis: During 2025, Kerala recorded 2,258 suspected cases and 3,469 confirmed cases, with 223 reported deaths. Flooding, poor drainage during the monsoon, and unsafe occupational exposures fuel recurrent outbreaks. Delayed diagnosis and critical care constraints contribute to high fatality rates, particularly in flood-prone districts.
- Nipah virus: Since 2018, Kerala has experienced multiple Nipah virus outbreaks. In 2025, the state reported 4 confirmed Nipah cases, including 2 deaths. The virus’s high fatality rate and outbreak potential underscore the need for sustained preventive measures, rapid emergency response mechanisms, adequate ICU capacity, and close coordination across human, animal, and environmental health sectors. Nipah virus is recognised by the WHO as a pathogen with epidemic and pandemic potential.
- Scrub typhus: In 2025, Kerala reported 158 suspected cases and 864 confirmed cases, resulting in 13 deaths. This mite-borne infection is expanding beyond rural pockets into urban and hilly regions. Delayed detection highlights gaps in diagnostics and fever case management, reinforcing the need for stronger primary care and surveillance systems.
Nutritional Health
- Anaemia: Anaemia remains a persistent public health issue in Kerala, especially among women and children. As per National Family Health Survey-5 (NFHS-5), over 30% of women of reproductive age are anaemic. This reflects ongoing gaps in iron supplementation, food diversity, and nutrition education.
- Vitamin deficiencies: Micronutrient deficiencies are widespread across age groups. As per the Comprehensive National Nutrition Survey (CNNS), nearly 27% of school-aged children show signs of vitamin A deficiency, and around 32% of adolescents and 12% of pre-schoolers have vitamin D deficiency. Vitamin B₁₂ deficiency affects nearly half of adolescents.
- Malnutrition: Kerala faces a dual burden of undernutrition and obesity. Around 23% of children are stunted, 16% are wasted, and 20% are underweight. At the same time, 4% of under-5 children and 38% of adult women are overweight or obese.
- Poverty and food insecurity as underlying determinants: Kerala still has around 5.9 lakh Antyodaya Anna Yojana households, indicating continued dependence on subsidised food systems.
- Dietary quality, affordability, and nutrition inequities: Limited dietary diversity and rising food prices disproportionately affect women, children, older adults, and tribal populations.
Mental Health
- Mental illness: An estimated 11.3% of the population experiences mental health conditions.
- Suicide: Kerala has one of the highest suicide rates in India—about 30.6 per 1 lakh population—with over 10,970 deaths reported in 2023.
- Substance use: Around 12.4% of the population consumes alcohol. In 2024, Kerala recorded 27,701 cases under the NDPS Act.
- Adolescent mental health: Over 60% of adolescents show symptoms of depression or anxiety. School-based mental health support remains severely inadequate.
Emerging Systemic Threats
- Antimicrobial Resistance (AMR): AMR is a growing public health threat. While Kerala has led containment efforts through KARSAP and Operation AMRITH, gaps remain in prescription oversight and OTC dispensing control.
Injuries and Trauma
- Road traffic injuries: In 2024, Kerala reported 48,919 road traffic accidents and 3,774 deaths. In 2025 (up to November), the state recorded 45,543 accidents and 3,365 deaths, underscoring ongoing pressure on trauma systems.
2.2 Infrastructure, System Resilience, and Governance
Gaps in Public Health Facilities
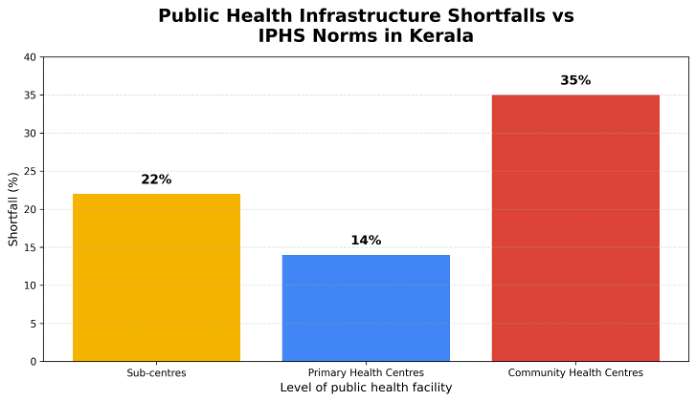
- Shortfall in primary care facilities: As highlighted in the CAG Performance Audit (2024), Kerala continues to face a substantial shortfall in frontline public health infrastructure. There is a 22% shortfall in Sub-Centres (SCs) and a 14% shortfall in Primary Health Centres (PHC) compared to prescribed norms. The deficit is more pronounced at the secondary level, with a 35% shortfall in Community Health Centres (CHC). Districts such as Malappuram and Idukki remain particularly under-served. Only two districts meet PHC norms and just one meets SC norms, revealing persistent geographic inequities in access to basic public healthcare. These infrastructure gaps leave rural, coastal, and remote populations with limited access to timely primary care, increasing avoidable referrals and dependence on higher-level facilities.
- Urban primary care: Despite Kerala’s strong aggregate health indicators, urban areas remain significantly underserved by the public primary care system. As of early 2025, the state has 102 Urban Primary Health Centres (UPHCs) and only 2 Urban Community Health Centres (UCHCs), covering just 58 of 93 urban local bodies. Over one-third of municipalities lack even a single UPHC. Only 29% of urban wards and 18% of the urban population are covered under the National Urban Health Mission (NUHM). This gap disproportionately affects urban poor, informal-sector households, and migrant workers, who are often compelled to rely on private clinics and hospitals for routine care, thereby increasing out-of-pocket expenditure even for minor ailments.
- Access gaps in tribal and remote areas: In tribal and hilly regions such as Attappady, public health infrastructure remains limited despite Kerala’s longstanding commitment to universal health coverage. The Attappady valley, home to approximately 30,000 tribal residents, is served by only two PHCs, one CHC, and a single Tribal Specialty Hospital. Most tribal hamlets lack even a sub-centre. In one widely reported instance, a pregnant woman was forced to be carried nearly 16 kilometres on foot, resulting in a stillbirth due to delayed access to care. These areas continue to face weak road connectivity, limited ambulance availability, and thinly staffed facilities, reflecting persistent structural neglect in health-system planning for geographically and socially vulnerable populations. People who suffer from emergencies due conditions such as accidents, heart attack, stroke or complicated delivery most often rush to private healthcare facilities in Coimbatore city in Tamil Nadu State disregarding the district-level tertiary care facilities at Palakkad town due to the bad condition of the roads to Palakkad. This causes out-of-pocket spending for the transportation and treatment. For visiting Attappady recently, it’s reported that, the health minister also avoided the Kerala roads and took the route via Coimbatore.
- Shortfall in secondary care facilities: The latest CAG Performance Audit shows serious shortfalls in secondary-care facilities. The Executive Summary records a 35% shortfall of CHCs compared with IPHS norms in the State. Of 5,332 health-infrastructure works approved during 2016–22, only 1,304 (24.45%) were completed; for secondary hospitals specifically, just 1 of 46 (CHC)/District Hospital (DH)/ Sub- District Hospital (SDH) – also called Taluk Hospital (THQH) works (2%) and 16 of 50 CHC works (32%) were completed, with the rest dropped or not started. In terms of beds, 16 of 19 District Hospitals had beds below IPHS norms and in 11 of these 16 DHs the deficiency was more than 40%. Many test-checked SDHs and CHCs lacked adequate or safe buildings, with some SDH buildings declared unsafe but still in use and several CHCs functioning from old or inadequate buildings, further weakening secondary-care service delivery.
- Shortfall in tertiary care facilities: The latest CAG Performance Audit report shows major shortfalls in tertiary care capacity. Of the new government medical college projects planned as tertiary centres, only one was fully completed by the cut-off date, while others remained around 70–90% complete, limiting the intended expansion of tertiary beds and services. In at least one medical college, only about 60–65% of sanctioned inpatient beds were operational due to incomplete buildings and support infrastructure. Critical tertiary units such as burns units, trauma/ICU facilities and key equipment (including sufficient functional ventilators) were either delayed, not fully equipped or non-functional, leading to under-utilisation of nominal ICU and specialty capacity. Trivandrum medical college, the first medical college in Kerala, face shortages in staff, beds, equipment, ICU facilities and even ventilators.
- Limited maternity and specialty services at local facilities: A large proportion of PHCs and CHCs lack the infrastructure, equipment, and trained personnel required to provide basic maternity care or essential specialist services. Consequently, more than 60% of deliveries in Kerala now take place in private hospitals, even when antenatal care has been provided through government facilities. This pattern reflects not only service limitations at public institutions but also declining public confidence in the availability of emergency obstetric care at local government facilities. The resulting shift towards private institutions significantly increases household expenditure on childbirth and postnatal care.
Hospital Capacity Constraints and Uneven Bed Distribution
- Unsafe and ageing public health infrastructure: A significant share of Kerala’s public health infrastructure is operating under unsafe conditions. Audit findings and official assessments have identified over 225 buildings across 134 government hospitals as structurally unsafe or at risk of failure.
- Overcrowding and bed shortages in tertiary hospitals: Kerala’s major public hospitals operate far beyond sanctioned capacity. For instance, the Medical College Hospital (MCH) in Thiruvananthapuram functions at over 170% occupancy.
- Long waits for treatment and critical care: Backlogs for surgeries and specialised procedures are common. At Thrissur medical college, more than 400 cardiac patients remain on waiting lists due to the presence of only a single active cardiac surgeon.
- Bed capacity meets national norms but lags behind needs: Though Kerala has a hospital bed ratio of approximately 1.2 beds per 1,000 population, it remains inadequate considering the morbidity pattern and health-seeking behaviour.
- Systemic referral issues exacerbating overcrowding: Weak coordination between primary, secondary, and tertiary facilities significantly contributes to congestion at medical colleges.
Fragile Emergency Care and Referral Transport Systems
- Gaps in trauma and emergency care infrastructure: Most government hospitals lack dedicated trauma care units or emergency surgery facilities.
- Referral transport and inter-facility coordination gaps: Families frequently bear the responsibility of moving patients between facilities due to inconsistent ambulance support.
- Limited emergency response capacity in the public sector: The ‘108 Kerala Emergency Medical Services Project (KEMP)’ faces persistent coverage gaps, particularly in rural, coastal, and hilly areas.
- Operational and funding challenges affecting ambulance services: By late 2024, unpaid dues led to state-wide strikes by ambulance personnel, disrupting services.
- Referral transport and inter-facility coordination gaps: Inefficient referral chains contribute to tertiary-level overcrowding and reliance on private emergency services.
Governance, Decentralisation, and Coordination Gaps
- Overlapping responsibilities and dual control: Kerala’s decentralised health system continues to suffer from blurred accountability between local governments and state-controlled staff.
- Underutilisation of Panchayati Raj Institutions (PRIs) and health funds: More than half of health-sector grants available to local bodies remained unutilised or delayed in use.
- Weak intersectoral coordination affecting disease prevention: Recent communicable disease outbreaks have highlighted gaps in coordinated action across departments.
- Budgetary and institutional rigidity limiting local action: Health accounted for about 5.5% of total state expenditure in 2024–25, limiting fiscal space for reform.
- Weak accountability, oversight, and implementation capacity: System audits have pointed to persistent governance failures in procurement and infrastructure management.
Limited integration of disaster preparedness within health governance: Kerala faces rising climate-related risks including floods, landslides, heat stress, and monsoon-linked disease outbreaks. District- and local-level health institutions vary widely in readiness, reflecting gaps in embedding disaster risk management within regular health governance processes.
2.3 Human Resources for Health
Health Workforce Gaps
- Staffing shortfalls across the system: Kerala’s public health system continues to face significant staffing gaps. While primary and secondary-level facilities maintain relatively better staffing, tertiary institutions such as medical colleges and specialty hospitals remain under-resourced. Specialist roles including gynaecologists, anaesthetists, and pathologists are commonly vacant in CHCs and DHs. Specialist and teaching posts in medical colleges showed large vacancies, with only about 30% to 80% of sanctioned posts filled in some institutions, effectively reducing the functional tertiary care capacity despite existing infrastructure as per the latest CAG report.
- Regional imbalance and rural access gaps: Health workforce distribution is uneven across the state. Northern districts like Kasaragod and Malappuram have below doctor-to-population ratios. Remote, hilly, and tribal areas continue to face persistent staffing challenges. Many villages lack Accredited Social Health Activists (ASHA), and several rural Primary Health Centres operate with only one doctor or remain unstaffed.
- Lack of a dedicated Public Health Management Cadre: Kerala has yet to implement a dedicated Public Health Management Cadre (PHMC), unlike states such as Tamil Nadu. In the absence of a specialised public health leadership structure, the system remains predominantly clinician-driven, limiting sustained focus on disease surveillance, prevention, and health-systems planning.
- Administrative and recruitment bottlenecks in health workforce management: Persistent workforce shortages in Kerala’s public health system are driven not only by workload pressures and migration, but also by prolonged recruitment and appointment delays. Recruitment through the Kerala State’s Public Service Commission (PSC) often involves extended timelines between notification, examination, rank list finalisation, and appointment, leaving sanctioned posts vacant for long periods, particularly in specialist and teaching cadres. Even where posts are approved, appointments are frequently slowed by procedural and fiscal clearances, including delays in finance concurrence and restrictions on regular recruitment. These systemic delays weaken timely workforce deployment and contribute to chronic staffing gaps across public health institutions.
- Reliance on contractual staff and ageing workforce: In response to delayed recruitment, public health institutions—especially medical colleges and specialty hospitals—have increasingly relied on contractual, deputation-based, and outsourced staff. While this provides short-term operational flexibility, it weakens institutional continuity and long-term workforce planning. At the same time, a significant proportion of senior staff is nearing retirement, raising concerns about leadership gaps and loss of institutional experience in public facilities.
- Overload, burnout, and migration pressures: Due to staffing shortages, many government facilities in Kerala are severely overburdened. Some hospitals operate with one nurse for every 50 to 60 beds, far below acceptable standards. This excessive workload contributes to burnout and fatigue among staff. Doctors experience high emotional exhaustion, depersonalisation, and a diminished sense of accomplishment, often working long hours with little time for personal life. These pressures have accelerated attrition and outward migration, particularly among nurses seeking better working conditions and remuneration abroad.
- Private sectors pull and limited retention incentives: The private sector employs a majority of the state’s medical professionals, especially specialists. Public sector jobs, particularly in underserved areas, often lack competitive compensation, career advancement opportunities, and supportive working conditions. Without targeted incentives for rural and remote postings, and improved human resource management, the state struggles to retain qualified staff in public facilities.
- Salary delays and dissatisfaction among frontline workers: Persistent delays in salary payments and low honoraria continue to demotivate frontline health workers. ASHA workers have repeatedly protested unpaid incentives and stagnant remuneration, while contractual and outsourced staff—including ambulance personnel and hospital support staff—have raised concerns over delayed wages and lack of job security. These issues disrupt service delivery and contribute to workforce instability.
- Gender-specific constraints and workplace safety concerns: Women healthcare workers face additional structural and social constraints. Safety concerns during night shifts, inadequate security arrangements, lack of safe transport, and insufficient workplace facilities remain widespread.
- Rising violence against healthcare workers: Incidents of violence against doctors and nurses have increased in recent years, including physical assaults and mob attacks in hospital settings. Though the Kerala Healthcare Service Persons and Healthcare Service Institutions (Prevention of Violence & Damage to Property) Act, 2012, has been amended in 2023 to strengthen legal protections, enforcement remains uneven.
Medical Education Gaps
- Expansion of intake without commensurate postgraduate training: Kerala by the academic year 2025 to 2026 has 5,150, with nearly 1,850 of these in government medical colleges. The increase in the number of medical seats in the past has occurred without a formal needs assessment. Nursing education has expanded to nearly 10,000 BSc seats, the majority of which are in private institutions. Allied health sciences including pharmacy, laboratory technology, and physiotherapy also enrol several thousand students annually. However, the seats for postgraduate courses and specialty training, particularly within government institutions, is not matched with the expansion of undergraduate seats. This shortage is applicable for medical, paramedical, and other assistive technology courses.
- Infrastructure and faculty constraints in training institutions: Many medical and nursing colleges continue to face faculty shortages, with more than 15 percent of posts remaining vacant in several government institutions. Some newly established medical colleges operate without independent campuses and rely on shared infrastructure in district hospitals. In nursing education, regulatory bodies require colleges to be affiliated with large hospitals, but inspections and approvals often lag. Several institutions have admitted students without meeting necessary infrastructure or regulatory benchmarks.
- Limited public health education and career pathways: Despite Kerala’s complex public health needs, the state faces gaps in public health education and workforce capacity. Formal training programmes such as Master of Public Health (MPH), health management, and epidemiology remain limited in number, uneven in quality, and weakly linked to the public health system. More critically, the absence of clearly defined career pathways for trained public health professionals within the public sector leads to underutilisation of expertise and discourages young professionals from entering or remaining in the field. As a result, key public health functions at district and state levels are often managed through ad hoc arrangements or clinical cadres without specialised training, weakening evidence-based decision-making and limiting the state’s ability to address emerging challenges such as ageing, non-communicable diseases, climate-linked risks, and outbreak preparedness.
- Challenges in quality assurance and regulation: Despite regulatory oversight, maintaining uniform quality across institutions remains difficult. Some private colleges bypass accreditation protocols or operate without full faculty strength. Students in certain institutions may lack access to adequate clinical exposure, laboratory facilities, and mentorship, raising concerns about the consistency of training quality.
- Gaps in curriculum and specialization: Curricula across many institutions remain heavily theoretical, with insufficient emphasis on clinical skills and applied public health. Specialties like Emergency Medicine, Family Medicine, Geriatrics, and Sports Medicine remain underdeveloped. Skill labs, continuing education, and public health field exposure are often underutilized, particularly in private institutions.
- Over centralisation of medical education and research governance: Kerala’s medical and allied health education system is highly centralised. Over 290 institutions operate under a single university, Kerala University of Health Sciences (KUHS) and regulatory framework without adequate vision or infrastructure that commensurate with the modern ethos of medical education. This concentration of authority has limited institutional autonomy, slowed curriculum updates, and constrained region-specific training and research priorities. Delays in faculty recruitment, approvals for new courses, and research funding allocations have further reduced system agility. The absence of multiple autonomous academic and research hubs has weakened innovation, restricted competition, and reduced the capacity of medical education institutions to respond effectively to Kerala’s evolving health and workforce needs.
- Absence of a state medical research board: Kerala lacks a standalone statutory Medical Research Board to set and govern state health research priorities. While institutions such as the KUHS and agencies under the Kerala State Council for Science, Technology & Environment (KSCSTE) support research, there is no central body aligning research with the state’s epidemiological needs. Existing mechanisms to translate research into clinical and policy action remain limited, and funding for research of wider relevance appears inadequate. The Kerala Health Research and Welfare Society (KHRWS) exists as a government society focused on hospital services and diagnostics but does not function as a central health research governance body.
2.4 Drugs, Vaccines, Diagnostics, and Technology Systems
Diagnostic and Laboratory Infrastructure Gaps
- Absence of basic diagnostics at primary and secondary levels: Despite infrastructure upgrades, a significant number of Family Health Centres (FHCs) and PHCs lack functional laboratories due to shortages of lab technicians, equipment, or consumables. Recent audit findings show that 1 in 4 upgraded PHCs had no laboratory services, while many CHCs and Taluk hospitals lacked essential diagnostics such as X-ray, ultrasound, Electrocardiogram (ECG), and routine biochemistry tests contrary to IPHS norms. Patients are routinely referred to higher centres or private laboratories for investigations, delaying diagnosis and increasing out-of-pocket expenditure.
- Disproportionate concentration of advanced diagnostics in tertiary hospitals: Advanced imaging (CT, MRI) and specialised laboratory services (histopathology, microbiology, oncology diagnostics) are available primarily in medical colleges and a small number of district hospitals. Only a handful of district/general hospitals have Computed Tomography (CT) or Magnetic Resonance Imaging (MRI) facilities, resulting in routine referrals from peripheral hospitals to medical colleges. This creates diagnostic bottlenecks, long waiting periods, and avoidable overload of tertiary institutions additionally contributing to gender inequity in accessing care.
- Equipment shortages, downtime, and maintenance failures: Even where diagnostic equipment exists, frequent breakdowns and delayed repairs significantly reduce functional availability. Procurement and maintenance systems remain weak, with limited annual maintenance coverage and delayed replacement of ageing machines. In 2024, budget reallocations led to a reported cut of over 40% in funds originally earmarked for upgrading laboratories and blood banks, directly affecting diagnostic capacity. As a result, patients are often advised to seek tests privately or wait extended periods for critical investigations.
Drugs Stock-outs and Fragile Supply Chains
- Widespread stock-outs of essential medicines: Public facilities continue to experience frequent shortages of essential drugs, including medicines for diabetes, hypertension, cardiac emergencies, infections, and anaphylaxis. A recent audit documented over 62,000 instances of drug stock-outs in public hospitals over a multi-year period, with delays extending from several months to multiple years for certain medicines. These shortages disrupt chronic disease management and emergency care.
- Delayed procurement and weak supplier accountability: Centralised procurement through Kerala Medical Services Corporation Ltd (KMSCL) has faced persistent delays, with over 80% of drug orders supplied late in recent audit cycles. Penalty clauses for delayed delivery and non-compliance have been inconsistently enforced, weakening supply reliability and accountability.
- Quality assurance and inventory management gaps: Audit findings have flagged instances of expired medicines being issued and inadequate batch-level quality testing. Poor forecasting, acceptance of near-expiry stock, and weak digital inventory controls contribute to simultaneous wastage and shortages. These failures compromise patient safety and fuel public distrust in government-supplied medicines.
Vaccination Services and Logistics Challenges
- Shortages of essential vaccines and biologics: Kerala experienced intermittent shortages of critical vaccines and biologics between 2023 and 2025. A major example was the acute shortage of Equine Rabies Immunoglobulin (ERIG) in 2023, when government hospitals—including tertiary medical colleges—ran out of ERIG required for high-risk dog-bite cases. While intradermal rabies vaccines were available, procurement delays and administrative lapses disrupted ERIG supply, forcing hospitals to arrange costly local purchases and exposing patients to treatment delays. In 2024, shortages of hepatitis B vaccine were reported, affecting new-born immunisation in private hospitals which also demonstrated inadequate coordination of the government with the private sector. These episodes highlight vulnerabilities in vaccine forecasting, procurement, and supply-chain governance.
- Recurrent rabies fatalities despite vaccine availability: Kerala continues to report preventable human rabies deaths despite the availability of effective vaccines and established treatment protocols. State data indicate 15 deaths in 2022, 17 in 2023, and 22 in 2024, with some fatalities occurring even after post-exposure vaccination. These cases point to gaps in timely access to rabies immunoglobulin, wound management, protocol adherence, and follow-up care. Weak stray dog population control, inconsistent animal birth control implementation, and poor coordination between health, veterinary, and local government systems further undermine prevention efforts.
- Persistent immunisation coverage gaps in vulnerable populations: Although overall immunisation coverage in Kerala remains high, significant sub-state inequities persist. Certain districts continue to report lower full-immunisation rates, leading to outbreaks of vaccine-preventable diseases such as measles. Tribal communities face particular challenges, with studies showing full immunisation rates among tribal children substantially below the state average due to access barriers, limited awareness, and follow-up dropouts. Children of migrant workers are another vulnerable group, often missing routine vaccinations because of frequent mobility, documentation barriers, and limited engagement with local health systems. These coverage gaps increase outbreak risks and undermine herd immunity.
- Cold-chain logistics and vaccine storage weaknesses: Maintaining vaccine potency remains a challenge due to operational gaps in cold-chain management. While Kerala has adopted modern cold-chain monitoring systems, lapses in adherence to protocols continue to occur. Equipment failures, power interruptions, inadequate backup arrangements, and insufficient supervision have resulted in vaccine wastage incidents and risks of administering compromised doses. Last-mile delivery to remote, hilly, and tribal areas further strains cold-chain integrity, especially during adverse weather conditions.
- Fragmented digital immunisation records and data use limitations: Kerala’s transition to digital immunisation platforms has improved visibility but introduced new challenges. Multiple systems for beneficiary tracking, vaccine inventory, and programme reporting continue to operate in parallel, leading to duplication of data entry and inconsistencies. During the rollout of newer digital registries, frontline workers faced constraints in training, connectivity, and workload resulting in delayed or incomplete data entry. Legacy paper records and partial migration of historical data have further limited the reliability of digital immunisation databases. Although digital tools have expanded coverage tracking, limited interoperability and under-analysis of data continue to constrain identification of coverage gaps and targeted planning.
Procurement and Regulatory Bottlenecks
- Rigid and slow procurement processes: Highly centralised and rule-bound procurement procedures delay timely purchase of medicines, diagnostics, and equipment. Hospitals have limited autonomy and unrealistic capping of local procurement to address urgent shortages or equipment failures.
- Weak enforcement of contracts and standards: Supplier accountability mechanisms such as penalties for delayed delivery or substandard quality have been inconsistently applied. Regulatory oversight of diagnostic services, laboratory standards, and biomedical equipment maintenance within public facilities remains uneven.
- Under-utilisation of allocated resources: Delays in approvals and tender finalisation have led to partial utilisation or diversion of funds earmarked for diagnostics, laboratories, and health technologies, reducing system readiness despite budgetary allocations.
Fragmented Digital Health and Information Systems
- Incomplete rollout of eHealth and electronic health records: Kerala’s e-Health initiative has expanded steadily but remains incomplete. As of 2024–25, around 1,000 public health facilities, approximately 44% of government institutions, were covered, leaving more than half still dependent on manual records. Continuity of care during referrals remains weak, as patient records are not universally accessible across facilities.
- Siloed and non-interoperable digital platforms: Hospital management systems, disease surveillance platforms, programme databases, and supply-chain software operate in silos with limited interoperability. The absence of a unified, real-time health data dashboard covering the entire state limits system-wide monitoring, outbreak preparedness, and resource planning.
- Under-utilisation of health data for decision-making: Although large volumes of health data are collected, they are often stored as static reports or Portable Document Formats (PDFs) and not analysed in real time. Disaggregated data on equity, geography, and vulnerable populations remain under-used. Weak integration between public and private sector data further constrains evidence-based planning and early warning systems.
Technology Gaps in Rural and Tribal Health Services
- Persistent digital connectivity deficits: Many rural and tribal health facilities face unreliable electricity and internet connectivity, limiting use of e-Health systems, telemedicine, and real-time reporting. Hundreds of tribal hamlets remain outside stable mobile or broadband coverage, restricting last-mile digital health delivery.
- Limited penetration of telemedicine and digital outreach: Teleconsultation platforms and mobile health initiatives exist but remain unevenly deployed in hilly and tribal regions due to infrastructure gaps, device availability, and digital literacy constraints among providers and patients.
- Dependence on episodic outreach and mobile services: Mobile clinics and pilot technology-enabled programmes have improved access in some tribal areas, but coverage remains intermittent. Lack of stable, technology-supported primary care infrastructure limits continuity of care for vulnerable populations.
2.5 Service Delivery and Quality of Care
Uneven Service Delivery, Regional Inequities, and Access Gaps
- Inconsistent staffing and service readiness across facilities: Public health facilities in Kerala show wide variation in service delivery capacity due to uneven staffing and operational readiness. Recent audits report doctor shortages across all levels of care, with specialist gaps most pronounced at secondary and tertiary facilities. District-level disparities persist, with northern districts recording lower doctor-to-population ratios. In many facilities, outpatient staffing does not align with patient load, resulting in long waiting times and overburdened providers.
- Variable service packages and minimum standards compliance: Many public hospitals do not consistently deliver the “minimum essential services” mandated under IPHS. Even among FHCs upgraded under the Aardram Mission, intended service improvements have not been uniformly realised due to staffing and operational constraints. As a result, patients experience significant variation in available services depending on facility type and location.
- Geographic inequities in quality of care: Kerala’s public health network is extensive, but effective access and service quality vary significantly by geography. Public healthcare utilisation remains higher in rural Kerala (approximately 42–43%) than in urban areas (around 34%), reflecting greater rural dependence on government facilities. However, rural users more frequently face delays due to limited access to specialists, diagnostics, and follow-up services, driving referrals and additional out-of-pocket costs. Rural CHCs and facilities in northern Kerala often provide fewer services and lower-quality care than better-performing counterparts elsewhere. As of 2025, only a limited number of CHCs had achieved national quality certification, indicating that most remain below benchmark.
- Persistent disadvantage in tribal, coastal, and remote regions: Tribal regions, including Attappady and parts of Wayanad, continue to face higher barriers to timely care due to difficult terrain, scattered hamlets, transport constraints, and weak continuity of services. Evidence highlights significantly poorer health and nutritional indicators in tribal communities, including underweight prevalence of around 46% and anaemia levels of approximately 10%, demonstrating that Kerala’s strong aggregate indicators mask deep pockets of deprivation. Coastal and fishing communities experience discontinuous access due to occupational mobility, rigid facility timings, and wage-linked opportunity costs. Delayed diagnosis and interrupted follow-up for chronic diseases are common, even when public consultations and medicines are available.
- Diagnostics access and quality as a service delivery constraint: Despite clinical consultations being available, many patients are forced to move across facilities—or rely on private laboratories—for even basic diagnostic tests, delaying diagnosis and treatment. The CAG report (2024) noted that several PHCs and CHCs lacked functional diagnostic services on all working days, resulting in external referrals for routine investigations. Weak diagnostic stewardship—marked by inconsistent quality assurance, inappropriate or repeated testing, and limited feedback to clinicians—undermines clinical decision-making. These gaps contribute to fragmented care journeys, higher OOPE, and avoidable referrals to private or higher-level facilities.
- Hospital-acquired infections (HAI) and patient safety surveillance: Surveillance of hospital-acquired infections (HAI) remains weak and fragmented. Recent state-level reviews indicate that only a minority of public hospitals conduct regular, documented audits of nosocomial infections. Infection control committees exist on paper in most facilities, but routine data reporting on Surgical Site Infections (SSI), catheter-associated infections, and neonatal sepsis is inconsistent. Public hospitals continue to report outbreaks of severe postnatal and post-operative infections, suggesting gaps in sterilisation protocols, overcrowding-related risks, and limited accountability mechanisms. The absence of systematic infection surveillance and public reporting undermines patient safety and erodes trust in institutional care.
- Limited public–private collaboration: The large private health sector operates with minimal coordination or oversight from the public system. Though Kerala has demonstrated successful projects of public–private partnership (PPP) in national programmes for addressing diseases such as TB, HIV and Polio, the state lacks equivalent PPP interventions in engaging private hospitals and clinics in the remaining areas of healthcare provision.
- Traditional and alternative medicine: Ayurveda, Yoga and Naturopathy, Unani, Siddha, Homeopathy (AYUSH) services run in parallel to the modern medicine system with little coordination. Referrals or co-management between modern and AYUSH providers are rare, resulting in fragmented care pathways for patients who utilize both systems.
Fragmented Care Pathways and Weak Continuity
- Weak gatekeeping and referral inefficiencies: Primary care does not function effectively as the first point of contact for many conditions, particularly chronic diseases such as diabetes and hypertension. As a result, patients frequently bypass PHCs and CHCs and directly access medical colleges and tertiary hospitals, contributing to a steadily increasing patient load, overcrowding of outpatient services, longer waiting times, and diversion of tertiary resources away from complex and referral-appropriate care. In parallel, a significant proportion of patients seek care directly from private clinics and hospitals, driven by perceived quality and faster access to diagnostics and specialists, which in turn leads to high OOPE even for conditions that could be managed at the primary-care level. Referral systems largely operate as one-way transfers, with limited advance communication, weak referral documentation, and minimal feedback from higher-level facilities to referring centres, resulting in poor continuity of care, duplication of investigations, and inefficient use of secondary and tertiary health services.
- Absence of back-referral and follow-up mechanisms: There is no robust system to track referred patients or ensure their return to primary care after stabilisation. PHCs seldom receive feedback from secondary or tertiary hospitals, and discharged patients are not proactively recalled. These gaps severely weaken continuity of care for chronic illnesses, post-hospitalisation recovery, and emergency follow-up.
- Siloed vertical programmes limiting integrated care: Major health programmes—covering non-communicable diseases, communicable diseases, mental health, and maternal–child health—often function as parallel verticals with separate reporting and service delivery arrangements. Patients with multiple conditions navigate fragmented pathways, attending different clinics and providers without coordinated care plans.
- Public–private fragmentation in the care continuum: Public and private providers operate largely in parallel, with no integrated referral tracking, shared medical records, or continuity protocols. State insurance schemes facilitate private-sector treatment, but coordination and quality oversight remain limited. Patients frequently move between sectors, leading to duplication of services, inconsistent treatment plans, and higher out-of-pocket expenditure.
- Prescription practices and pharmacy accountability: Inappropriate prescribing remains a systemic concern. State drug-control inspections and audit findings indicate widespread non-compliance with prescription-only regulations, particularly for antibiotics and high-risk medicines. Antibiotics continue to be dispensed without valid prescriptions across a large share of retail pharmacies, contributing to rising antimicrobial resistance. Prescription audits in public facilities remain sporadic, and digital prescription monitoring is not yet universal. These gaps weaken rational drug use, increase treatment failures, and add to avoidable household expenditure.
- Limited monitoring of quality and outcomes under public insurance schemes: While Karunya Arogya Suraksha Padhathi (KASP) and Pradhan Mantri Jan Arogya Yojana (PMJAY) have expanded access to private-sector care, systematic quality oversight remains weak. Available grievance data show that a significant proportion of complaints relate to denial of services, informal payments, and incomplete coverage of diagnostics and medicines. National PMJAY reviews indicate that only a small fraction of empanelled hospitals undergo regular quality audits, and outcome indicators such as complication rates or readmissions are not routinely tracked or disclosed. As a result, patients, particularly those with complex conditions, experience variable quality of care despite being insured.
- Cancer care equity concerns despite insurance coverage: Cancer patients in Kerala continue to face geographic and financial inequities. Studies indicate that nearly half of cancer patients travel over 50 km for treatment, disproportionately affecting rural and low-income households. Even among insured patients, out-of-pocket expenditure remains substantial—driven by diagnostics, medicines, and radiation therapy not fully covered under insurance packages. This contributes to delayed treatment initiation and unequal outcomes.
Variable Quality Standards, Equity, and Patient Experience
- Inconsistent application of clinical protocols: Adherence to standard treatment guidelines varies widely across public facilities. Audit findings highlight gaps in infection control, antenatal care protocols, and emergency procedures. Only 10% of procured drug batches are routinely quality tested, allowing large volumes of medicines to be used without laboratory verification. Equipment maintenance practices are irregular, affecting service reliability and patient safety.
- Partial coverage of quality assurance mechanisms: Kerala has expanded quality initiatives, with around 240 public facilities accredited under National Quality Assurance Standards (NQAS) by mid-2025, alongside Labour Room Quality Improvement initiative (LaQshya) and Making Unique Services Quality Assured for children (MUSQAN) certifications for maternity and child-friendly services. However, most facilities remain outside formal accreditation, and routine enforcement of quality standards remains weak. Although Kerala enacted its own Clinical Establishments (Registration and Regulation) Act, 2018 to regulate hospitals and clinics, full implementation of regulatory mechanisms—including inspection and enforcement—has been slow and uneven, and application of minimum standards under the Act has not yet been consistently enforced across the state.
- Programme-level quality gaps in key population groups: Continuity and quality of care remain uneven in priority areas. NCD services show variable follow-up and case management across districts, contributing to high out-of-pocket spending. Community mental health services remain underdeveloped, with limited integration into primary care. Elderly care services lag behind demographic needs, despite rapid population ageing. In maternal and child health, audits note uneven uptake of entitlement schemes, even as select facilities demonstrate high-quality care through certification programmes.
- Unequal quality of care for marginalised and special populations: Despite universal service intent, care quality and continuity remain uneven for marginalised groups. Scheduled Castes (SCs) and Scheduled Tribes (STs) experience higher unmet need due to geographic isolation, limited outreach, and uneven service quality, with women and children particularly vulnerable. Migrant workers face language barriers, documentation challenges, and episodic engagement with public health services, often limited to disease surveillance rather than continuous care. Fisherfolk encounter rigid service timings and wage-linked barriers to follow-up. Persons with disabilities face persistent physical and communication barriers—facility audits show that while ramps exist in many centres, fewer than 40% of public facilities are fully accessible. Transgender persons continue to report stigma, lack of trained providers, and inconsistent implementation of inclusive care policies. These patterns reflect a “one-size-fits-all” service design that fails to adapt to diverse social and occupational realities.
- Weak data-driven quality monitoring and feedback loops: Health system data are insufficiently disaggregated by district, gender, disability, social group, or migration status, limiting the detection of inequities in care quality and outcomes. There is no institutionalised mechanism for routine outcome audits, equity reviews, or public reporting of service quality indicators. Although grievance redress systems exist, reviews show that complaints are poorly categorised and rarely linked to corrective action or provider accountability, allowing systemic quality gaps to persist.
Maternal, New-born, and Early Childhood Care Quality Gaps
- Maternity care and patient experience deficits: While Kerala reports institutional delivery rates exceeding 99%, quality of maternity care remains uneven. Patient grievance records and facility-level audits indicate persistent instances of suboptimal maternity care, including inadequate communication, limited informed consent for obstetric interventions, and insufficient emotional support during labour and delivery. These experiences undermine trust in public facilities and disproportionately affect first-time mothers and socially vulnerable women.
- Antenatal workforce constraints: Auxiliary Nurse Midwives (ANMs) and nurses with midwifery training are critical providers of community-based antenatal care, tasked with antenatal monitoring, counselling, and risk identification. Yet, coverage and utilisation of these services remain uneven, particularly among marginalised populations. Recent analyses raise concerns about a reduced emphasis on dedicated midwifery roles and skill sets, resulting in gaps in continuity of care at the community level—especially for high-risk pregnancies. These workforce constraints weaken early detection of complications, weaken follow-up support, and reduce the effectiveness of preventive maternal care, underscoring the need for strengthened workforce capacity, enhanced training, and sustained antenatal engagement across communities.
- High caesarean section rates and post-operative safety risks: Kerala records one of the highest caesarean-section rates in India, exceeding 45% overall and crossing 60% in private hospitals—far above WHO-recommended thresholds. Public hospitals increasingly report post-caesarean complications, including surgical site infections and puerperal sepsis, contributing to avoidable maternal morbidity and ICU admissions. These trends point to gaps in infection prevention practices, post-operative monitoring, staffing adequacy, and clinical quality oversight in obstetric services.
- Limited early intervention for autism and neurodevelopmental disorders: Children with autism spectrum disorder and other neurodevelopmental conditions face significant delays and service gaps in the public health system. Limited specialist availability and capacity constraints result in long waiting periods for diagnosis and therapy at government facilities. Comprehensive developmental services are concentrated in a small number of tertiary centres, which are already overstretched. Consequently, many families turn to private providers for speech, behavioural, and occupational therapy. Private therapy costs range from ₹500 to ₹1,500 per session, imposing substantial financial strain on households requiring long-term care. The lack of affordable, decentralised early intervention services leads to delayed treatment during critical developmental periods and increases inequity in access to care.
2.6 Financial Protection and Affordability
Limited Financial Protection under Public Insurance and Public Provisioning
- Limited effective insurance coverage: While 51.5% of households in Kerala have at least one member covered by some form of health insurance (NFHS-5), most of this protection comes from publicly funded schemes such as KASP and Ayushman Bharat, which offer limited coverage focused mainly on select hospitalisations. Private health insurance remains limited and socially skewed, concentrated largely among salaried professionals and high-income households. For the majority of informal workers, self-employed households, elderly populations, and those living with chronic illness, private insurance remains either unaffordable or inaccessible.
- Narrow coverage and ‘hidden costs’ despite insurance: Kerala’s publicly funded insurance architecture—primarily AB-PMJAY and the state-run Karunya Arogya Suraksha Padhathi (KASP)—formally empanels over 500 hospitals, including nearly 200 government facilities and more than 300 private hospitals. It largely covers inpatient hospitalisation, while outpatient consultations, diagnostics, medicines, transport, food, and follow-up care remain inadequately covered. As a result, insured families continue to incur substantial expenses. One state analysis found median private-hospital admission spending of approximately ₹9,000 among insured patients, compared to ₹10,500 among the uninsured—indicating only marginal reduction in financial burden once indirect and uncovered costs are considered. Awareness gaps, administrative complexity, and digital barriers further limit effective utilisation among informal workers and marginalised groups.
- Persistently high out-of-pocket spending: Kerala continues to report among the highest out-of-pocket (OOP) health spending burdens in the country. Recent health accounts estimate indicate that households in Kerala continue to finance around 59.1% of total health expenditure out of pocket. Even within public services, costs accumulate through travel, medicines procured outside government supply chains, and external diagnostics. Recent survey data show that average out-of-pocket spending per hospitalised household in Kerala stands at approximately ₹8,655 in rural areas and ₹10,341 in urban areas—substantially higher than national averages. This indicates continued erosion of financial protection even for patients accessing public-sector hospital care.
- Fiscal stress and scheme sustainability risks: Kerala has expanded insurance coverage beyond centrally supported beneficiary limits, increasing fiscal pressure. The state has covered roughly 42 lakh vulnerable families, while the centrally recognised pool is around 24 lakhs. Since 2019, hospitals reportedly provided about ₹4,700 crore worth of treatment under the scheme while central contribution was around ₹778 crore, leaving the state to finance approximately ₹3,920 crore. According to data presented in the state assembly, there is a financial backlog of nearly ₹2,000 crore in pending dues to both government and private hospitals — with over ₹1,700 crore owed under KASP alone, including more than ₹376 crore to private hospitals — raising concerns about timely reimbursements and continuity of care for beneficiaries under these schemes.
- Service denial and provider exit due to payment arrears: Persistent reimbursement delays have translated into access constraints in practice. By early 2025, empanelled hospitals reported over ₹1,300 crore in pending claims, prompting several private hospitals to halt or discourage admissions under public insurance schemes. This has reduced effective provider choice for beneficiaries and forced insured patients to either pay privately or travel farther for care, weakening the real-world value of insurance coverage. At the same time, public hospitals have faced growing financial strain, with unpaid claims affecting procurement of medicines, consumables, and diagnostic services, and increasing pressure on already constrained operational budgets. Together, these dynamics have reduced effective provider choice for beneficiaries and forced insured patients to either pay privately, rely on overstretched public facilities, or travel farther for care—weakening the real-world value and credibility of insurance coverage.
- Under-priced benefit packages and incomplete financial risk pooling: Insurance benefit packages have not been periodically revised to reflect rising healthcare costs. Several procedures remain under-covered, and package rates are widely viewed by providers as financially unviable. This contributes to informal charges, claim disputes, and reluctance to admit insured patients, particularly for complex or high-cost conditions. As a result, large segments of the population continue to face substantial financial exposure despite nominal insurance coverage.
Unequal Impact of Health Expenditure on Vulnerable Households
- Catastrophic spending concentrated among the poor: Evidence shows that catastrophic health expenditure is disproportionately borne by poorer urban households, with a substantially higher share of low-income families experiencing health spending which is estimated as 17% of household consumption. This highlights persistent inequality in financial protection, even within a health system that performs well on many aggregate indicators.
- Chronic illness amplifying financial vulnerability: Long-term conditions impose sustained financial strain on households. Dialysis demand has increased sharply in Kerala (from 44,000 patients in 2020 to over 2.1 lakh by 2024), while interruptions in insurance payments and limited public capacity push many patients towards private providers. Recurrent monthly expenses for dialysis, medicines, and transport remain catastrophic for economically disadvantaged families, contributing to debt, distress financing, and treatment discontinuation.
- Cost-related care rationing and delayed care-seeking: Transport expenses, wage loss, and the cost of medicines and diagnostics discourage early care-seeking and regular follow-up. Vulnerable groups including migrants, fisherfolk, tribal households, persons with disabilities, and the elderly often delay tests, skip follow-ups, or seek care only during emergencies. These behaviours increase disease severity, treatment costs, and long-term health risks, reinforcing cycles of vulnerability.
- The ‘missing middle’ remains inadequately protected: Beyond the poorest households covered by public insurance, a substantial “missing middle” remains exposed—too well-off to qualify for government schemes, yet unable to afford private insurance or absorb medical shocks. This group faces full financial risk for hospitalisation and chronic care, contributing to widening inequities in financial protection.
Gaps in Entitlement Awareness and Effective Coverage
- Health literacy and community engagement deficits: Despite high general literacy levels, health literacy remains uneven across populations. Surveys indicate that a significant share of eligible households lack clarity on insurance entitlements, benefit packages, referral pathways, and grievance mechanisms. Digital-only enrolment and claims processes pose barriers for elderly persons, migrants, and low-income households. Community engagement mechanisms—such as participatory planning, feedback forums, and health education outreach—remain weak or unevenly implemented, reducing effective uptake of entitlements and financial protection schemes.
- Strong schemes, uneven reach and utilisation: Kerala operates multiple entitlement and assistance mechanisms, including insurance schemes, benevolent funds, and disease-specific support. Some initiatives demonstrate scale and capacity—for instance, dialysis support in public facilities has been reported at approximately 50,000 sessions per month across major government centres. However, awareness, documentation requirements, and uneven local implementation limit effective reach, particularly among informal workers, migrants, and less-educated households.
- Implementation fragility due to funding and operational delays: Even when services are officially designated as “free,” continuity is vulnerable to funding delays and supply disruptions. A recent example involved interruption of supplies in a home-based dialysis support programme due to pending dues of around ₹7 crore, leading to rationing and restrictions in service provision. Such disruptions reduce predictability, weaken trust in public schemes, and force households to seek costly private alternatives.
Barriers for Vulnerable Groups
- Migrant workers excluded: Kerala’s large interstate migrant workforce remains largely outside effective financial protection. Recent assessments indicate that around 86% of migrant workers are unaware of state health schemes, and only about 10% report having any form of health insurance. Language barriers, lack of documentation, and weak targeted outreach mean that even eligible individuals are often unable to enrol or utilise benefits, leaving them exposed to high health-related financial risk.
- Disabled persons under-covered: Persons with disabilities face both limited entitlements and serious implementation gaps. Kerala operates a dedicated disability insurance scheme with coverage up to ₹1 lakh and provides disability pensions, but recent years have seen major disruptions. In 2024, reimbursements under the disability insurance programme were halted, affecting over three lakh beneficiaries. State social welfare payments—including disability pensions and caregiver stipends—have faced prolonged delays, resulting in arrears running into several hundred crore rupees. Monthly disability pensions of ₹1,600 went unpaid for extended periods, forcing many beneficiaries to pay insurance premiums and treatment costs out of pocket, effectively nullifying financial protection.
- Elderly lack access: Kerala’s senior citizen healthcare programme is predominantly urban-centred and chronically underfunded. In 2024, unpaid dues led to the reduction of the programme’s medicine list from about 130 items to 85, including the removal of essential drugs such as insulin. Over 3 lakh elderly persons depend on this programme, many of whom are now compelled to purchase medicines privately. Funding shortages have also suspended mobile clinics and outreach services, particularly affecting poor and remote elderly households.
- Tribal and marginalised communities: Indigenous and marginalised communities continue to face persistent access gaps despite formal coverage. Special tribal health initiatives provide free tertiary care and limited non-medical support in high-burden areas, yet utilisation of institutional services remains low. Field assessments indicate that culturally insensitive care, experiences of discrimination, long travel distances, and the need to leave familiar environments discourage many tribal families from seeking treatment. As a result, although services are formally free, practical and social barriers prevent effective access, particularly for maternal, child, and chronic care.
Structural Drivers Undermining Financial Protection
- Low public health spending relative to need: Kerala’s health spending remains modest by its own high standards. The 2024–25 state budget allocated approximately 5.5% of total expenditure to health, which is below the average share seen in several other states and short of the National Health Policy’s recommendation that states progressively increase health’s budgetary share towards around 8% of total expenditure. Chronic under-investment in health infrastructure and services undermines system capacity, pushing households towards private care and higher out-of-pocket costs.
- Constrained fiscal health and competing budget priorities: Kerala’s broader fiscal health context constrains its ability to prioritise public health amid competing budgetary demands. According to NITI Aayog’s Fiscal Health Index (FHI) 2025, Kerala scored 25.4 and ranked 15th out of 18 major states, placing it among the lower-performing states in overall fiscal health. The assessment highlights persistent weaknesses in quality of expenditure and debt sustainability, despite relatively strong own-revenue mobilisation. A high share of routine and committed expenditures, coupled with low capital spending, reduces fiscal space for developmental outlays, including sustained investment in health infrastructure and programme expansion. In this constrained fiscal environment, public health funding competes with other obligations, limiting the state’s ability to scale up preventive, primary, and tertiary care even as demographic transitions and disease burdens intensify.
- Weak regulation of private healthcare costs: Oversight of private healthcare pricing remains limited. Although the Clinical Establishments Act was enacted to standardise charges, implementation has lagged. As of 2025, many facilities still do not transparently display rates or adhere to standard pricing norms. In practice, private hospitals retain significant discretion to levy additional charges, leaving even insured patients vulnerable to unexpected bills. Without stronger enforcement and price regulation, financial protection through insurance remains partial and uneven.
- Commercialisation and corporate expansion of healthcare: Kerala has experienced rapid corporatisation of healthcare, with large private hospital chains expanding through mergers, acquisitions, and private equity investment. Corporate hospitals account for a growing share of tertiary and quaternary care, particularly in oncology, cardiology, and organ transplantation. This expansion has coincided with rising treatment costs, higher diagnostic intensity, and increasing out-of-pocket spending, even among insured patients. Private-sector charges for common procedures have risen faster than insurance package revisions, encouraging informal billing and balance payments. Profit-driven care models increasingly shape treatment decisions, weakening affordability and complicating effective regulation.
2.7 The Invisible Backbone of Kerala’s Health System
AYUSH
- Parallel systems with poor integration: Kerala has a strong presence of AYUSH practitioners, but they largely operate in silos apart from the allopathic system. There is little coordination or referral between modern medicine and AYUSH services – patients often navigate the two systems on their own, resulting in fragmented care pathways and missed opportunities for comprehensive treatment.
- Under-resourced public AYUSH facilities: The government runs Ayurveda hospitals, dispensaries, and homeopathy clinics, yet many of these face staff and infrastructure shortfalls. Key positions (specialist doctors, therapists) may remain vacant, and facilities often lack medicines or equipment. In some remote areas, an AYUSH practitioner might be the only health provider available, but without integration and adequate support, their ability to handle complex conditions or emergencies is limited.
- Regulatory and quality control gaps: While there are councils and regulations for AYUSH, enforcement of standards can be uneven. The quality assurance for AYUSH medicines and therapies is not as rigorous or uniform as in modern medicine. Variability in training across institutions means skill levels differ, and there is ongoing debate about efficacy and safety which has not been fully addressed through research or updated protocols, potentially undermining public confidence.
- Limited role in public health programmes: AYUSH systems have not been effectively woven into mainstream public health initiatives in Kerala. For instance, AYUSH doctors are typically not engaged in immunisation programmes, outbreak response teams, or national health missions in an integrated way. This exclusion means the health system is not capitalising on AYUSH practitioners’ community reach and preventive approach – a significant missed opportunity for holistic care and health promotion.
- Stagnant career structure and modernisation challenges: Career progression for AYUSH doctors in government service is narrow, often capped at running a small facility or moving into academia. There are few specialty training programmes to upgrade their expertise (e.g., in areas like panchakarma, yoga therapy, or research methodologies). Moreover, cross-training opportunities that foster collaboration with allopathic peers are rare. These factors lead to professional stagnation and maintain a divide between traditional and modern systems, instead of a collaborative healthcare model.
- Weak digitalisation, data use, and documentation systems: Platforms like Ayush Health Information Management System (AHIMS) have low uptake and limited interoperability with mainstream digital health platforms like e-Health and Ayushman Bharat Digital Mission (ABDM). Most institutions still rely on parallel paper systems, hindering data-driven planning, outcome tracking, and system integration.
- Supply-chain vulnerabilities and medicine quality issues: State-run production units have faced licensing delays and periodic disruption in drug manufacturing, affecting continuity of supply to public AYUSH facilities. The lack of dedicated testing infrastructure—such as for homoeopathic drug quality—limits pharmacovigilance and undermines public trust.
- Lack of defined roles in chronic care, mental health, and rehabilitation: Although AYUSH systems are suited to long-term management, wellness, and preventive care, there are no structured pathways for their participation in areas like palliative care, post-acute rehabilitation, or mental health. As a result, their contribution remains peripheral despite system needs.
Nurses
- Chronic nurse shortages and heavy workloads: Many public hospitals face severe nursing shortfalls, with some wards operating at unsafe nurse-to-patient ratios (e.g. one nurse per 50+ patients). Overstretched staff experience burnout and fatigue, compromising care quality and driving nurses to seek better opportunities elsewhere.
- Uneven distribution and vacancy delays: Nursing personnel are concentrated in urban centres and private facilities, while rural and remote areas struggle to recruit and retain staff. Lengthy hiring processes and reliance on temporary contract nurses leave sanctioned posts unfilled for long periods, exacerbating regional gaps in care.
- Limited career pathways and recognition: Professional advancement for nurses is constrained, with few leadership roles or specialist positions available. Despite being the frontline caregivers, nurses have minimal say in policy decisions and limited avenues for growth, leading to low morale.
- Training and skill-mix issues: The rapid expansion of nursing education – largely in the private sector – has led to variable training quality. New graduates often lack adequate practical exposure in critical care, geriatrics, and other emerging areas. In-service training and continuous skill upgradation remain sporadic, leaving some nurses ill-prepared for evolving healthcare needs.
- Workplace safety and gender concerns: The predominantly female nursing workforce faces safety challenges at work. Inadequate security during night shifts, lack of safe transport, and occasional incidents of harassment or violence in hospital settings add stress. These unresolved safety issues contribute to job dissatisfaction and deter entrants to the profession.
ASHAs
- Coverage gaps in vulnerable areas: Certain villages and tribal pockets remain without an Accredited Social Health Activist (ASHA) or equivalent community health worker. These gaps in frontline coverage mean essential services – door-step health education, basic newborn care, follow-ups for TB or antenatal cases – can be uneven, leaving high-need communities underserved.
- Low pay and delayed incentives: ASHAs receive only a modest honorarium and task-based incentives, which are frequently delayed. This persistent financial insecurity, with no fixed salary or benefits, leads to frustration. Many ASHAs have staged protests over unpaid dues and stagnant remuneration, reflecting deep dissatisfaction at the grassroots level.
- Overburdened and at risk of burnout: ASHAs juggle multiple duties – from immunisation drives and disease surveillance to accompanying patients to hospitals – often covering large populations with minimal support. The mounting workload and pressure to meet targets without adequate tools or rest lead to stress and burnout among these workers.
- Lack of training and career progression: Initial training for ASHAs is brief, and opportunities for refresher courses or new skills are limited. There is no clear career pathway for community health volunteers to move into higher positions (such as becoming ANMs or supervisors). This absence of upward mobility and professional development causes stagnation and attrition.
- Integration and support challenges: While ASHAs are the vital link between communities and the health system, they often operate in isolation. Supervision is patchy – regular support visits and feedback are inconsistent – and ASHAs have little authority to ensure referred patients actually receive care. Insufficient integration into the primary care team and lack of transport or safety provisions hinder their effectiveness on the ground.
Allied Health Professionals and Paramedics
- Undervalued support roles in the system: Allied health professionals (lab technicians, radiographers, physiotherapists, etc.) and emergency paramedics are essential for diagnostics, rehabilitation, and emergency response, yet they receive limited policy attention. These critical support roles often remain invisible in health planning, leading to ad hoc deployment and neglect of their needs.
- Staffing shortages and maldistribution: Many public hospitals and health centres face shortages of allied health staff. Vacant posts for lab techs, X-ray technicians, physiotherapists and other technicians are common, impairing service delivery. Urban tertiary hospitals tend to have more full-fledged allied teams, whereas rural facilities often operate without key technical personnel, reflecting uneven distribution.
- Outsourcing and job insecurity: In the absence of regular recruitment, numerous allied health and paramedic positions are filled via contract or outsourcing (for example, ambulance Emergency Medical Technicians (EMTs) or lab services on contract). These workers often have lower pay, no benefits, and little job security. High turnover and uncertainty weaken team cohesion and continuity of care in public institutions.
- Training and regulatory gaps: The quality of allied health education and certification is inconsistent. A proliferation of private training institutes has created a workforce with varying skill levels. Standardised curricula, licensing, and regulatory oversight for many allied professions are still emerging, resulting in uneven competencies and practice standards across the state.
- Limited career growth and integration: Career pathways for allied health workers are ill-defined. A lab technician or therapy assistant often remains in the same role for years with few chances for promotion or specialization. Moreover, these professionals are seldom included in higher-level decision making or multidisciplinary case discussions, leading to underutilisation of their expertise and low morale.
Pharmacists
- Inadequate staffing and workload pressure: Each government primary health facility typically has only one pharmacist who must manage hundreds of prescriptions daily. This mismatch between workforce and workload – rooted in outdated staffing norms – results in long patient wait times, overwhelmed staff, and greater risk of dispensing errors.
- Slow recruitment and reliance on temporary staff: Pharmacist posts have not expanded in line with service needs. Even as patient volumes and medicine lists grow, the creation of new permanent posts is sluggish. To fill gaps, the system leans on short-term hires (e.g. contract pharmacists during specific programmes or crises), which is a stopgap solution and leaves many facilities chronically understaffed.
- Underutilised clinical skills: Pharmacists are trained in medication therapy and counselling, but in practice their role in Kerala’s public sector is confined mostly to dispensing. There is little integration of pharmacists into clinical teams or public health initiatives, meaning the system misses out on their potential contributions to rational drug use and patient education.
- Limited professional development: Opportunities for pharmacists to update skills or advance professionally are scarce. There are few specialised training programs (for example in clinical pharmacy, toxicology, or hospital pharmacy management) and a lack of clear promotion avenues beyond the basic pharmacist role. This stagnation can diminish motivation and contribute to pharmacists leaving for the private sector.
- Regulatory and practice challenges: Enforcement of pharmacy regulations remains patchy. Instances of medicines being dispensed without proper prescriptions persist in the retail sector, putting pressure on pharmacists to balance patient demands with legal guidelines. In public facilities, pharmacists often handle inventory and administrative burdens without adequate support, diverting time from patient-focused services and complicating quality assurance.
Dental and Oral Health Workforce
- Minimal public provision of oral healthcare: Oral health has long been sidelined in Kerala’s public system. Only a small fraction of dentists are employed in government facilities (just a few at community or district hospitals), leaving primary care without any dental services. As a result, most people depend on private dentists for even basic care, leading to high out-of-pocket costs and unmet dental needs among those who cannot afford private treatment.
- Urban-centric distribution: Dental professionals and clinics are heavily concentrated in cities and large towns, whereas rural and remote populations have scarce access to dental care. Many rural residents delay or forgo dental treatment due to distance and cost. This urban-rural imbalance contributes to a high burden of untreated dental caries, gum disease, and oral cancers in under-served areas.
- Workforce–needs mismatch: Kerala produces a large number of dental graduates annually, but public sector absorption is very limited. There are few sanctioned posts for dentists at primary or secondary care levels, leading to an oversupply of dentists competing for urban private practice jobs while government dispensaries and health centres lack oral health personnel. This misalignment signals a policy gap in leveraging the available dental workforce for public health.
- Lack of integration into health programmes: Oral health is not well integrated into general health initiatives. School health programs, community NCD screenings, and primary health outreach rarely include dental check-ups or oral cancer screenings. Dental teams are seldom part of multidisciplinary health camps or prevention drives. This siloed approach means missed opportunities for early detection of oral health issues and education on oral hygiene as part of routine healthcare.
- Career and infrastructure challenges: Dentists in the public system face slow career progression and often have to work with limited infrastructure. Dental units in government facilities may lack modern equipment or sufficient supplies, affecting service quality. Furthermore, there is a shortage of auxiliary dental workers (such as dental hygienists or dental assistants) in public health, and few programs to continuously train the oral health workforce in the latest techniques or community dentistry, hindering expansion of preventive services.
Public Health Professionals
- Undefined cadre and unclear roles: Kerala lack a clearly designated public health cadre with defined responsibilities. Medical officers often double up as program managers without adequate training in epidemiology, health systems, or data-driven planning.
- Shortage of trained public health personnel: There is a limited pool of MPH/Doctor of Medicine (MD) (Community Medicine) graduates in the system, and even fewer occupy frontline leadership positions in district surveillance units, programme management cells, or field epidemiology teams.
- Limited integration across programmes and departments: Public health functions like disease surveillance, vector control, health promotion, and outbreak response remain fragmented across vertical programmes, with weak coordination between departments and poor data convergence.
- Underinvestment in analytics and data governance: Despite Kerala’s e-Health investments, public health professionals are under-equipped to use data for planning or early warning. Training in Geographic Information System (GIS), modelling, or data analytics is rare, and routine health intelligence units remain underdeveloped.
- Weak public health leadership pipeline: There are few institutional pathways to identify, mentor, and retain public health leadership. Existing professionals face poor career progression, lack of recognition, and few incentives compared to clinical specialists.
- Neglected roles in emergency preparedness and climate resilience: As Kerala faces increasing climate-linked health threats (vector-borne diseases, heat stress, floods), the absence of strong public health leadership at local levels weakens risk planning, community preparedness, and adaptive response.
- Home
- Purpose And Scope
- Executive Summary
- 1. Introduction
- 2. Key Challenges and Gaps in Kerala’s Health System
- 2.1 Disease Burden and Emerging Health Risks
- 2.2 Infrastructure, System Resilience, and Governance
- 2.3 Human Resources for Health
- 2.4 Drugs, Vaccines, Diagnostics, and Technology Systems
- 2.5 Service Delivery and Quality of Care
- 2.6 Financial Protection and Affordability
- 2.7 The Invisible Backbone of Kerala’s Health System
- 3. Towards a People-Centred Health System: Setting the Direction for Reform
-
4. Recommendations for Health System Strengthening
- 4.1 Strengthen Infrastructure, Emergency Readiness, and System Resilience
- 4.2 Build a Strong, Modern Health Workforce & Improve Medical Education
- 4.3 Building Robust Systems for Medicines, Diagnostics & Technology Systems
- 4.4 Improve Service Delivery & Guarantee Quality of Care
- 4.5 Strengthen Governance, Financing, and Financial Protection
- 4.6 Build Strong Public Health Systems, Surveillance & Disease Preparedness
- 4.7 Strengthening the Invisible Backbone of Kerala’s Health Workforce
- 4.8 Transforming Key System Interfaces
- 5. Annexures
- Contributors

